

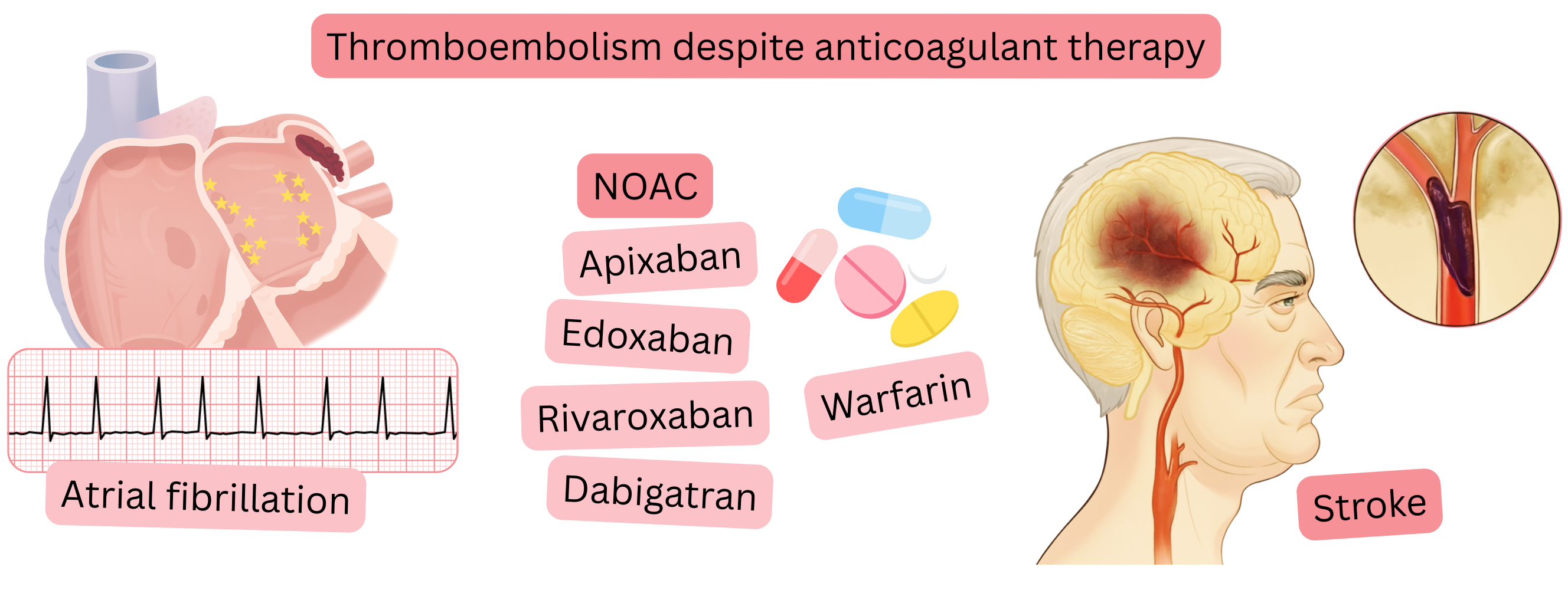
Oral anticoagulation therapy significantly reduces the risk of thromboembolism in patients with atrial fibrillation (AF).
Despite anticoagulation therapy, 30 % of patients with AF experience an ischaemic stroke. The main causes include:
For secondary prevention of recurrent stroke, the following may be considered:
| Thromboembolism and Atrial Fibrillation During Anticoagulation Therapy | Class |
|---|---|
| In a patient with atrial fibrillation (AF) receiving anticoagulation therapy who develops a stroke, comprehensive evaluation is recommended. | I |
| In a patient with AF receiving anticoagulation therapy who develops a stroke, switching anticoagulation therapy may be considered. | IIb |
| In a patient with AF receiving anticoagulation therapy who develops a stroke, adding antiplatelet therapy to anticoagulation may be considered. | IIb |
These guidelines are unofficial and do not represent formal guidelines issued by any professional cardiology society. They are intended for educational and informational purposes only.
